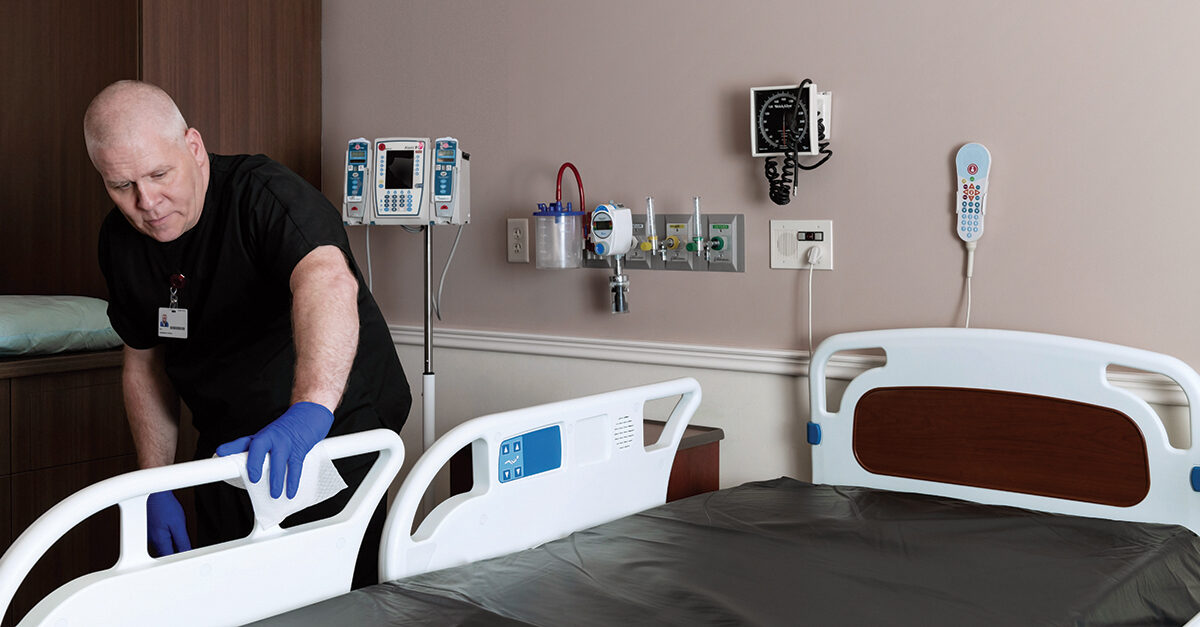
Patients can pick up health care-associated infections (HAIs), such as C. difficile and Methicillin-resistant Staphylococcus aureus (MRSA), in any health care facility, from hospitals and long-term care centers to doctors’ offices and ambulatory surgery centers. At any given time, about one in 25 patients has an HAI related to hospital care, according to the U.S. Department of Health and Human Services. As HAIs are caused by bacteria, fungi, viruses, and other pathogens that can live on surfaces, front-line cleaners and infection control specialists play an important role in preventing the spread of these germs.
Two specialists—Alice Brewer, director of Clinical Affairs for Tru-D® SmartUVC and Caitlin Stowe, the clinical affairs research manager for PDI Healthcare—answered questions CMM readers may have about adopting integrated infection control approaches in their facilities to reduce the number of HAIs.

Caitlin Stowe
Q: How prevalent are HAIs in the health care environment today and how do they impact the industry and patients?
Stowe: HAIs continue to be a significant issue today both in terms of patients’ health and costs to the industry. According to the U.S. Centers for Disease Control and Prevention (CDC), there are an estimated 687,000 HAIs each year, resulting in 72,000 deaths and costing an estimated US$11 billion. To put these numbers in perspective, HAIs kill more people each year in the United States than car accidents, breast cancer, or pneumonia.
Patients and health care professionals are vulnerable to a variety of infectious agents lurking throughout a hospital environment. The constant turnover of patients and the communicable nature of HAIs makes them pervasive. HAIs can also be quite persistent, with some outbreaks lasting for weeks, months, and even years. The good news is that there have been incredible advances and innovations in the industry to prevent and control HAIs. Health care in the United States is safer now than it was 10 years ago due to a steady decline in HAIs, according to the CDC.
Q: What types of products and interventions are currently in use to reduce the high incidence of HAIs?
Stowe: Modern health care facilities use an array of products and interventions to combat a wide spectrum of pathogens across the various sources and vectors of infections. HAIs are so pervasive because they can be transmitted through many sources, including health care workers’ hands, a patient’s skin, medical equipment and instruments, facility surfaces, and the overall environment. Products need to address each of these potential vectors.
Gloves, hand-sanitizing wipes, hand-sanitizer solutions, and soaps are key for reducing bacteria transmission from the hands of health care professionals. Washcloths, antiseptic wipes, and swabs/swab sticks are personal hygiene tools to remove pathogens from patients’ skin.
Strict cleaning and disinfecting protocols for floors, counters, furniture, linens, and other surfaces also are important for battling HAIs during daily and terminal cleanings and during total room disinfections. Effective products should have a wide antimicrobial spectrum, act quickly, and be nontoxic.

Alice Brewer
Q: What newer tools are being used for infection control and prevention and how effective are they?
Brewer: New innovations like automated, total room decontamination are growing in use across the industry and have been demonstrated in studies to be effective in battling HAIs. These technologies include vaporized hydrogen peroxide or mist (VHP or HPM), ultraviolet (UVC) light, and self-disinfecting surfaces. VHP/HPM works by using a portable generator to quickly increase the concentration of hydrogen peroxide available in the room for decontamination. UVC systems emit UVC wavelengths that are capable of inactivating microorganisms, such as bacteria, viruses and fungi, preventing them from replicating in the environment. Self-disinfecting surfaces are created by coating surfaces with heavy metals, germicides, or light-activated antimicrobials.
While more research is needed for self-disinfecting surfaces, studies published in Current Opinion in Infectious Diseases and the American Journal of Infection Control have shown that UVC and VHP/HPM are effective in reducing bacterial contamination of surfaces. Furthermore, studies published in The Lancet have specifically shown that a hospital adding a structured, targeted UV disinfection program to cleaning protocols, and maintaining a high compliance of manual cleaning, will likely have fewer incidences of C. difficile and vancomycin-resistant enterococcus (VRE).
Q: What are the benefits of manual cleaning versus automated? How do they complement each other?
Brewer: Manual cleaning and disinfection of hospital surfaces is critical for preventing infections and improving patient safety. The removal of dirt, debris, and organic material through the use of disinfecting products is crucial daily, as well as after a patient is discharged. Automated disinfection is an important second step for an effective infection prevention process.
Pathogens and germs can live anywhere and survive for months. Adding an automated technology, such as UVC, ensures the entire room is disinfected, including hard-to-reach and low-use areas. In fact, a recent study funded by the CDC, and published in The Lancet, showed enhanced terminal room disinfection with UVC reduced the relative risk of colonization and infection caused by epidemiologically important pathogens among patients admitted to the same room by 30% in hospital settings when performed 93% in compliance with standard disinfection protocols. It is important to note that individual hospital results may vary.
Q: Some health care facilities are moving to an integrated approach to infection prevention. What does this approach look like and what are best practices today in the clinical setting?
Stowe: An integrated approach in the health care environment incorporates protocols and products that address all the potential sources of transmission and contamination. This includes establishing a rigorous standardized set of policies such as strict handwashing, proper skin hygiene, thorough equipment disinfection or sterilization, and the use of appropriate cleaning and disinfecting products for daily and terminal cleaning as well as total room disinfection. The key to a successful integrated, layered approach is combining traditional “touch” cleaning and disinfecting with a “no-touch” automated system. Best practices include adopting organization-wide policies for all levels of employees to closely follow. Ensure all staff members undergo comprehensive education and training, then monitor their performance and encourage feedback.
Q: What are the potential benefits or shortcomings of an integrated approach to infection control?
Brewer: An integrated approach to infection control and prevention has many benefits for improving the safety of patients and health care professionals. As noted in the studies mentioned above, an integrated program provides effective, reliable, rapid, and safe decontamination activity against a wide range of health care-associated pathogens.
Automated technology, such as UVC, eliminates human error and is easy to use and transport. With UVC, for example, there are no chemicals or residue, and minimal health and safety concerns.
An integrated approach does require initial and ongoing capital costs for health care facilities, including an investment in technology, continuous training and monitoring of staff, and the implementation of communication policies that involve feedback. However, the cost savings associated with preventing infections, improving patient outcomes, and helping to save lives are certainly more significant.